| Journal of Medical Cases, ISSN 1923-4155 print, 1923-4163 online, Open Access |
| Article copyright, the authors; Journal compilation copyright, J Med Cases and Elmer Press Inc |
| Journal website http://www.journalmc.org |
Case Report
Volume 5, Number 1, January 2014, pages 1-3
Small Bowel Obstruction Due to Gastrointestinal Neurofibromas and Lipomas
Poul Guldfeldta, c, Rezvan Zardarib
aDepartment of Surgery, Hospital of Lillebaelt, Kolding, Denmark
bDepartment of Radiology, Hospital of Lillebaelt, Kolding, Denmark
cCorresponding author: Poul Guldfeldt, Lunde Bygade 58, 5450 Otterup, Denmark
Manuscript accepted for publication November 8, 2013
Short title: Small Bowel Obstruction
doi: https://doi.org/10.4021/jmc1579w
| Abstract | ▴Top |
The most known manifestation of neurofibromatosis Recklinghausen NF-1 is cafe-au-lait spots on the skin, but up to 25% of patients with NF-1 have gastrointestinal manifestations, and only 5% of the gastrointestinal manifestations of NF-1 will require surgical treatment. We report a rare case of a 73-year-old woman, who five times earlier has undergone bowel resection, due to intussusception and ileus. The patient was admitted to the hospital due to abdominal pain. A computed tomography scan showed progression of the almost disseminated tumor growth of neurofibromas and lipomas of the small intestinal wall. Clinical manifestions showed the ileus required an operative treatment with a sixth small bowel resection. Small bowl obstruction caused by neurofibromas is a rare manifestation of a rare disease.
Keywords: Neurofibromatosis Recklinghausen; Small bowl obstruction; Ileus; Intussusception
| Introduction | ▴Top |
Neurofibromatosis Recklinghausen (neurofibromatosis type 1, NF-1) is an autosomal dominant disorder with a prevalence of 1 per 4,000 individuals [1]. The most known manifestation of NF-1 is cafe-au-lait spots on the skin, but the disease can also appear in the form of cutaneous neurofibromas and irishamartomas [2]. In up to 25% of patients with NF-1, there are gastrointestinal manifestations. These gastrointestinal manifestations primarily affect the ventricle and small intestine. Gastrointestinal NF-1 has three different versions: visceral vasculopathy, diffuse ganglioneumatosis, and solitary neurogenic tumores [2]. The diffuse ganglioneumatose can present themselves as a tumor process containing ganglion cells, Schwann cells or fibroblasts [2]. Only 5% of the gastrointestinal manifestations of NF-1 will require surgical treatment [2].
Complications of the gastrointestinal neurofibromas are rare. The most frequent complications are ulceration, bleeding, and obstruction. More rarely, on case by case basis, there have been reported intussusception and perforation [3].
The changes are mostly of a benign nature and most often cause mechanical symptoms, but in 10-15%, the gastrointestinal neurofibromas can undergo a malignant transformation [2].
According to international diagnostic criteria for NF-1, which can be seen in Table 1, patients must have two or more of the symptoms in order to make the final diagnosis [4].
 Click to view | Table 1. At Least Two of the Following Seven Criteria Must be Present in Order to Make the Final Diagnosis of NF-1 |
Another gastrointestinal tumor process that macroscopic and radiologic may be difficult to distinguish from neurofibromas is lipomas.
Lipomas represents 5% of all gastrointestinal tumors and 10% of the benign gastrointestinal tumors. Lipomas in the gastrointestinal tract is usually located just beneath the mucosa and is usually asymptomatic, but may lead to obstruction, intussusception or bleeding. Lipomas can occur together with neurofibromas and is an important differential diagnosis [5].
| Case Report | ▴Top |
A 73-year-old woman is hospitalized due to increasing abdominal pain through 1 week. The patient’s medical record reveals that she suffers from intestinal neurofibromatosis. She has undergone small bowl resection five times since 1981, due to intussusception caused by neurofibromas in the small intestine.
The pathology reports of the previous resections have all shown neurofibromas.
A computed tomography scan performed at admission revealed disseminated tumor growth of neurofibromas, and lipomas of the small intestinal wall. Parts of the small intestine were dilated up to 8.5 cm before an intussusception in the left iliacal fossa (Fig. 1).
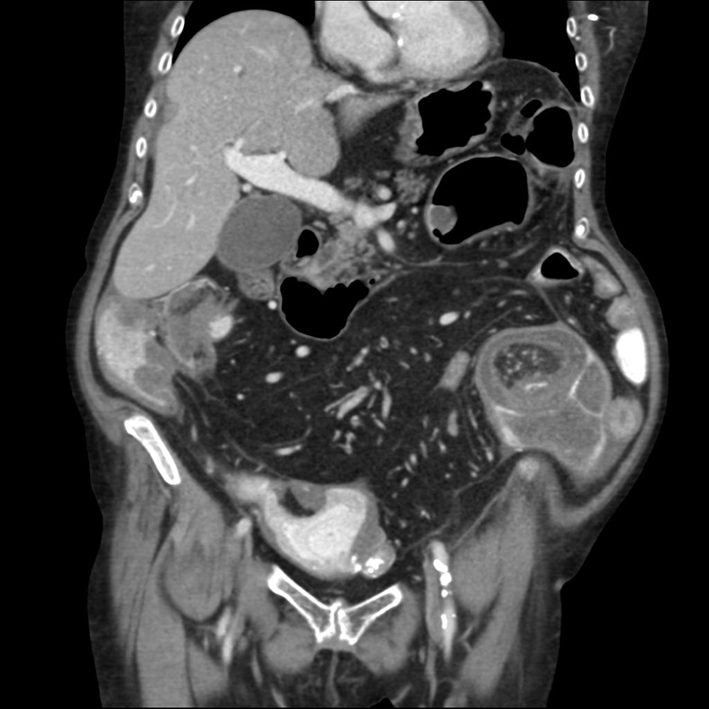 Click for large image | Figure 1. CT scan with oral contrast shows submucosa in the entire small intestine infiltrated by lipomas and neurofibromas. In the left iliac fossa there is an intussusception leading to obstruction. |
The patient’s medical condition continued to deteriorate and due to both clinical symptoms of bowel obstruction and the radiological findings, it was decided that an explorative laparotomy was needed. Intra-operatively an intussusception was found 1.5 m from the Treitz ligament, and one by an old ilio-colic anastomosis. There were two resections of the small intestine, both approximately 15 cm. Two primary anastomosis were made.
Because of rising infection parameters on the third postoperative day, antibiotic treatment with metronidazole and cefuroxime was started. Antibiotics was discontinued on the sixth postoperative day, because of declining infection parameters and normalization of temperature.
The pathology report from this latest operation describes tissue transformation compatible with intestinal neurofibromatosis and multiple lipomas.
| Discussion | ▴Top |
NF-1 is a relatively rare disease and gastrointestinal manifestations with symptoms that require surgical treatment are even more rare. Since this patient had previously been operated for the same condition, a new episode of ileus was suspected on admission to the hospital.
In the previous pathology reports, there are described neurofibromas in the removed parts of the small intestine. The pathology report from this admission also describes changes consistent with gastrointestinal neurofibromatosis.
Hence this patient has undergone bowel resection five times previously on the basis of intussusception and ileus caused by intestinal neurofibromas, there is nothing sinister in that she was admitted under the same picture again.
Small bowl obstruction caused by neurofibromas is, however, a rare manifestation of a rare disease. The instructive part in this story is that benign gastrointestinal tumor processes can result in ileus in the same way as a malignant tumor can. It is also notable that gastrointestinal neurofibromatosis can present itself with such massive growth of neufibromas as seen in Fig. 1. One should be cautious about bowel resection and only perform it on vital indication if the patient has such widespread changes in the abdomen as this patient, since there will probably come another episode of intussusception and ileus.
Conflicts of Interest
No conflicts of interest to declare.
Grant Support
No grant support.
| References | ▴Top |
- Ferner RE. Neurofibromatosis 1 and neurofibromatosis 2: a twenty first century perspective. Lancet Neurol. 2007;6(4):340-351.
doi - Fuller CE, Williams GT. Gastrointestinal manifestations of type 1 neurofibromatosis (von Recklinghausen's disease). Histopathology. 1991;19(1):1-11.
doi - Lie AK, Lindboe CF, Tommerup N, Johnsen G. [Gastrointestinal manifestations in neurofibromatosis]. Tidsskr Nor Laegeforen. 1993;113(4):454-456.
pubmed - Ruud E. [Neurofibromatosis 1—so easy to diagnose, but so difficult?]. Tidsskr Nor Laegeforen. 2002;122(25):2484.
pubmed - Balamoun H, Doughan S. Ileal lipoma - a rare cause of ileocolic intussusception in adults: Case report and literature review. World J Gastrointest Surg. 2011;3(1):13-15.
doi pubmed
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Journal of Medical Cases is published by Elmer Press Inc.


