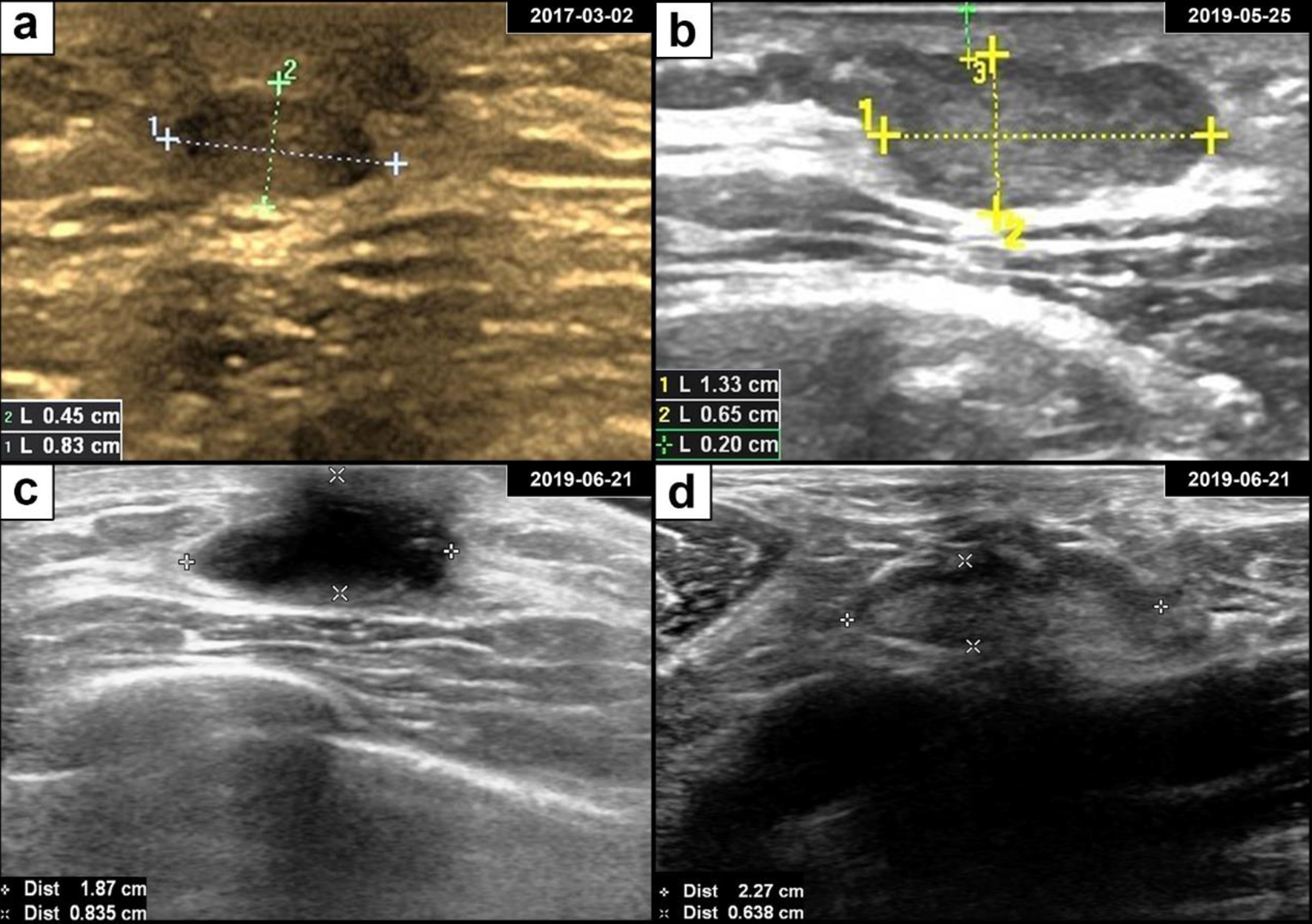
Figure 1. Breast adenoid cystic carcinoma ultrasound and postoperative findings. (a) Ultrasonography revealed a well-defined oval hypoechoic mass in the retroareolar region of the left breast. (b) The subareolar mass progressively enlarged over the course of 2 years. (c) Ultrasonography showed a hypoechoic area after lumpectomy. (d) Ultrasonography of an enlarged axillary lymph node with a clear boundary.
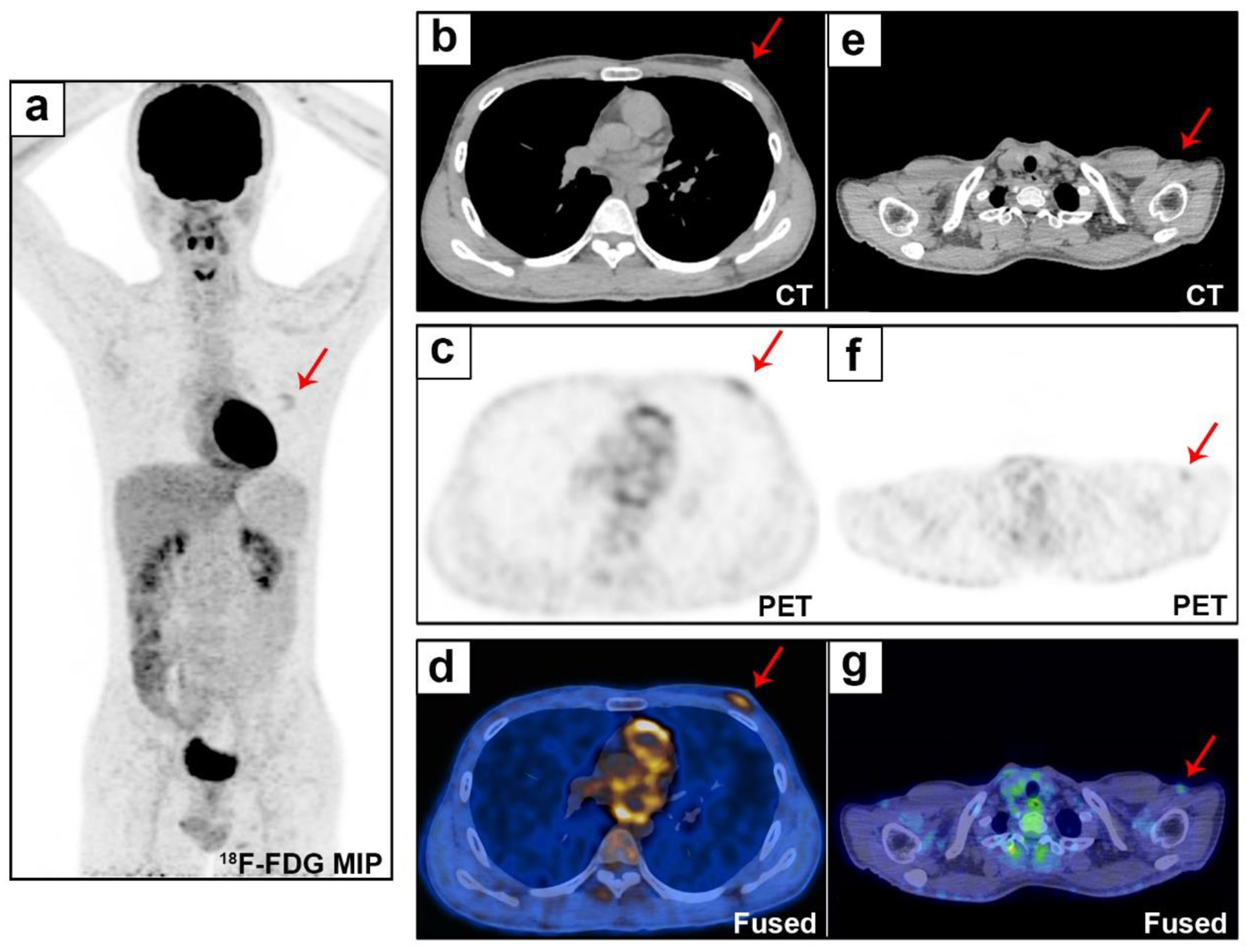
Figure 3. Whole-body evaluation by 18F-FDG PET/CT. The 18F-FDG PET/CT MIP (a) shows uptake (SUVmax 2.5) in the left breast lesion (b and d, red arrows), with a disordered tissue structure (c, red arrow). Small lymph nodes were found in the bilateral neck and bilateral axillary regions (e-g, red arrows, SUVmax 1.65). 18F-FDG PET/CT: 18F-fluorodeoxyglucose positron emission tomography/computed tomography; MIP: maximum intensity projection; SUVmax: maximum standardized uptake value.